TherapyThere is no specialized therapy for Locked-In-Syndrome, however practicing an intensive combination of physiotherapy, speech and occupational therapy has been approved.Generally it is proven that all therapies that attach great importance to concentration on the cognitive (consciousness-moderation) connection between perception and movement are suitable treatments. The earliest possible beginning of an intensive treatment in regards to therapy and mobilisation is extremely important. Experience has shown that the success of the rehabilitation depends directly on the time of the beginning respectively the beginning is strongly connected with it, meaning, the earlier patients begin with therapy measures, the more comprehensively and lastingly the success will be. But one needs to be aware that the intensity and duration of the treatment will quickly decrease as soon as the patient leaves the stationary phase. That is why we can only advice our patients to stay as long as possible under stationary treatment and we cannot endorse an early release. The LIS association supports afflicted people with the enforcement of this knowledge towards sponsors through its consultation and publication of scientific results. Therapy as much and as fast as possible! Therapie so viel und so schnell wie möglich! The therapy is divides in 3 parts: Paralyzed - what now? Physiotherapy is the most important measure to fight against a high-grade paralyzation. Though there are different ways of procedure. Today it is demanded that the therapy needs to be evidence-based, meaning, the need to be based on the newest practical and theoretical knowledge. There are still not a lot of therapy studies yet that have examined the success of the different practices. However, it turned out that they are effective in different ways and they might develop their optimal effect only in certain stages of the illness. In the following it is particularly dealt with the first phase of a severe paralyzation. In order to live independently we need our muscles that allow us all different kinds of movement. At the same time they must enable us to hold positions against the force of gravity, resistances and external weights. Therefore our brain plans in each case the necessary work orders, which are conveyed from different parts of the brain over different nerve tracts to the muscles. Nerve impulses for movements come mainly from the cerebral cortex. In contrast, orders for maintaining body positions come primarily from deeper brain sections as well as from joints, skin and muscles. Those nerve connections are developed after a firm, genetically steered plan at the beginning of our life. First, the networks are developed, which allow us to move. So one muscle group (e.g. the flexors) can get the commands to contract (shorten) and their opponents (the extensors) to slack off (lengthen) simultaneously. That combination causes a (bending) movement. And only when it is assured that all muscles not only can receive work orders but also sufficient orders to relax, those certain nerve paths will be developed, which convey tension for posture, because only now the muscle contractions can be deliberately limited.
In daily life, most muscles are more or less constantly working to produce tension to secure body positions. Movements, on the other hand, are less frequent. And when a movement is difficult to perform, even more tension is planned. In contrast, movements without any tension for posture are extremely rare. So the nerve connections, which transfer the commands for muscle tension, would be faster developed then the ones for movement instructions, until finally the muscles can produce tension again. Since however there are still no transmission paths available for the command of relaxation, this kind of muscle activity can not be limited again. Therefore not a normal, but impairment-oriented behaviour could be important after a brain lesion, so that - as at the beginning of life - the nerve connections for the movement activity are initially built up. On this basis, a new therapy technique has been developed in recent years, the "systematic repetitive basic training" (7,8), which leads and supports the patient to such a repair-oriented behaviour. Simply put: Initially in each joint only individual movements without accompanying static contractions are carried out. The therapist supports these as much as necessary. Because only when the brain receives feedback that the action was successful changes in the nerve connections are initiated (9). Not until movements are again possible, meaning when muscles can be shortened but also lengthened again, are the control loops for posture will be activated. In a third step movements and posture will be combined to different actions. This procedure was examined in a study of stroke patients and the effectiveness could be confirmed (10,11). An individual case study with a patient with Locked-In-Syndrome showed that the SRBT can also be suitable for this type of illness (12,13). In cases of paralyzation, where no spontaneous healing appears in the first months, it takes approximately 6 months until first movement activities are noticeable and approximately 18 to 24 months until daily activities are possible. One condition is that the patient tries the movements performed in the therapy and that the therapist supports him very precisely but only as far as necessary. In the first phase any effort is forbidden, because it almost always leads to muscle tension. Daily practising - whereby a break on the weekend is possible - seems to be also a condition. Literature: 1. von Bernhardi R et al. What Is Neural Plasticity? Adv Exp Med Biol. 2017;1015:1 - 15. Christel Eickhof,
Definition of Occupational Therapy:
Occupational therapy accompanies, supports and enables humans, who are threatened with the limitation or restriction of everyday activities. Here it concerns, people within their environment being able to accomplish significant manipulation in the areas of self-sufficiency, production and free-time. Exertion is the therapeutic medium and also the goal of intervention accordingly.
Um die oben beschriebenen Ziele zu erreichen, greift der/die Ergotherapeut/in auf verschiedene Behandlungsansätze zurück, wie z.B. nach Perfetti, Bobath, Affolter, Johnston, Catillo Morales, Feldenkrais oder anderen. Marita Storim (Occupational therapist) 

Speech therapy: One needs to find an individual communication possibility and training together with the speech therapist.
1. Gulp training
2. Speak and voice therapy
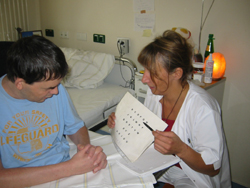 2. Locked-In patients suffer from a malfunction of speaking and voice, which is called dysarthria. Breathing, speaking and the movement of articulation organs can be impaired in the severe phase on account of the paralyzation, so that the patient cannot make himself verbally understood. The patient's speech system remains normally, so that contact can still be made through other ways of communication (e.g. concerted signals like one shut of the lids for 'yes', two for 'no', or letter tables). Purchasing and learning more complex appliances for a supported communication (e.g. LightWriter, Aladin, Tellus with MindExpress) might be a useful attachment, because regaining the verbal language requires a lot of time and effort.
The disordered areas are initiated and trained in the speech therapeutic treatment. Exercises that intensify the breath-in and lengthen the breath-out are very useful for example for breath training. Volume and modulation ability can be trained to support the voice. For some patients it is important e.g. to exercise the breech sounds and the soft palate function for a better understanding.
2. Locked-In patients suffer from a malfunction of speaking and voice, which is called dysarthria. Breathing, speaking and the movement of articulation organs can be impaired in the severe phase on account of the paralyzation, so that the patient cannot make himself verbally understood. The patient's speech system remains normally, so that contact can still be made through other ways of communication (e.g. concerted signals like one shut of the lids for 'yes', two for 'no', or letter tables). Purchasing and learning more complex appliances for a supported communication (e.g. LightWriter, Aladin, Tellus with MindExpress) might be a useful attachment, because regaining the verbal language requires a lot of time and effort.
The disordered areas are initiated and trained in the speech therapeutic treatment. Exercises that intensify the breath-in and lengthen the breath-out are very useful for example for breath training. Volume and modulation ability can be trained to support the voice. For some patients it is important e.g. to exercise the breech sounds and the soft palate function for a better understanding.
Frequent and aimed exercises are precondition for re-receiving the speaking ability. You can find addresses of therapists that give these treatments through the DBL or the association of breathing, speaking and voice teachers.
Frequency of the treatment::
Five times a week in the intensive phase; reducible to two to three times per week during the course. |
 Research done in the last years showed, however, that the brain of an adult is able to respond to new demands by changing its connections. This phenomenon is known as neuronal plasticity and associated with learning. (1) However, only actions that have been tried and were successful are learned.
Research done in the last years showed, however, that the brain of an adult is able to respond to new demands by changing its connections. This phenomenon is known as neuronal plasticity and associated with learning. (1) However, only actions that have been tried and were successful are learned.